- Get Certified
- Certification Process
- Subspecialties and FPDs
- Focused Practice Designations
- Anesthesiology Critical Care Medicine
- Emergency Medical Services (EMS)
- Health Care Administration, Leadership, & Management (HALM)
- Hospice and Palliative Medicine
- Internal Medicine – Critical Care Medicine
- Medical Toxicology
- Neurocritical Care
- Pain Medicine
- Pediatric Emergency Medicine
- Sports Medicine
- Undersea and Hyperbaric Medicine
Oral Exam
The Oral Certification Examination retired in 2025. ABEM has launched the Certifying Exam.
Learn more.
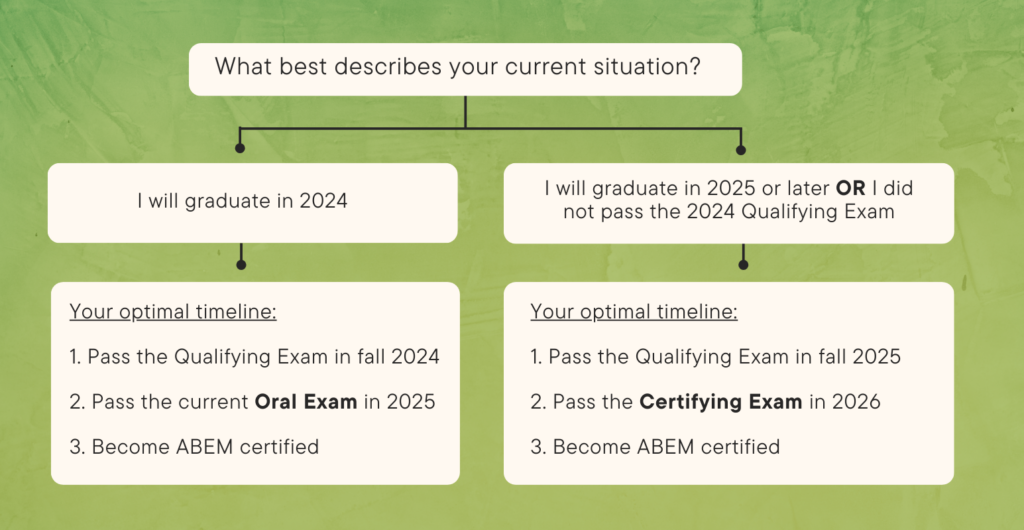
Will I take the Oral Exam or Certifying Exam?